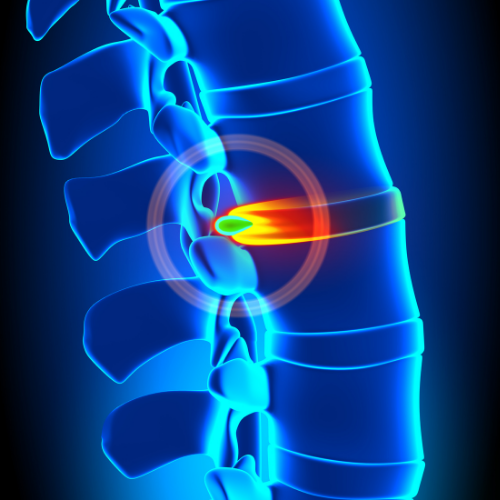
Cervical Degeneration is due to chronic and progressive arthritis of the cervical spine. The discs degenerate and cannot provide the cushion necessary to support the bones of the spine. As such, patients develop “bone-on-bone” between successive cervical bone levels and pain becomes the main complaint. As the discs degenerate, some patients can develop neck pain, shoulder pain, and even pain that radiates into the arms. Not all patients with cervical degeneration will develop neck pain or any symptoms for that matter. Smoking is certainly a factor that can worsen the progression of cervical degeneration even after having surgery. One of the risks for patients who undergo surgery is that the cervical spine continues to degenerate as you continue to age. Even though a patient may present with cervical degeneration and undergo successful treatment, they may have recurrent symptoms from another level over time. As the degeneration progresses, it can include foraminal stenosis around a nerve root leading to arm symptoms. Cervical degeneration can also develop into osteophytes that cause central Cervical Stenosis leading to Cervical Myelopathy. With central Cervical Stenosis, the spinal cord is compressed leading to hand numbness or weakness and with more progressive symptoms including difficulty with walking. Cervical degeneration usually occurs in patients after the age of 40 years old. Cervical Degeneration can be associated with a cervical disc herniation but not always. Some patients will present with an isolated cervical disc causing severe symptoms but not really have any Cervical Degeneration. Because Cervical Degeneration is most related to disc and bone deterioration, patients should have an X-Ray with flexion and extension views in addition to a CAT Scan and MRI of the cervical spine. MRI is more useful for soft tissue evaluation of the nerve and spinal cord whereas X-Ray and CAT Scan are better for bone and related osteophytes.
Cervical Degeneration
The Cervical Center is dedicated to the treatment and outcomes of patients who suffer from problems related to the cervical spine including any condition related to bone, nerve, or soft tissue. Our program is focused on high quality clinical outcomes and the most effective treatments for all conditions related to the cervical spine.